Acid Reflux Treatment
Acid Reflux (Gastro-Oesophageal Reflux Disease – GORD)
Patient Information
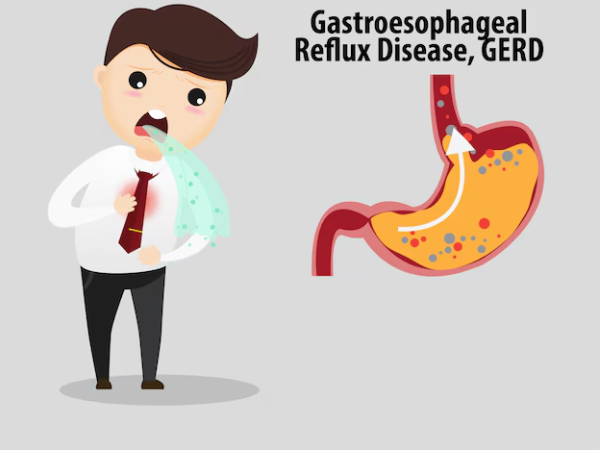
Acid reflux, also known as gastro oesophageal reflux disease (GORD),
is a common condition where stomach acid flows back into the oesophagus (food pipe). This can cause symptoms such as heartburn, regurgitation, chest discomfort, or throat irritation.
Many people experience occasional reflux. GORD is diagnosed when symptoms are recurrent, persistent, or affecting quality of life, or when complications develop.
What Causes Acid Reflux?
Acid reflux occurs when the valve between the oesophagus and stomach (the lower oesophageal sphincter) does not function effectively. This allows stomach contents to reflux upwards.
Factors that contribute include:
Weakening of the lower oesophageal sphincter
Hiatal hernia
Obesity or increased abdominal pressure
Pregnancy
Certain foods and drinks (e.g. fatty foods, alcohol, caffeine)
Smoking
Some medications
In many patients, reflux has more than one contributing factor.
Common Symptoms of Acid Reflux
Symptoms vary between individuals and may include:
Heartburn (burning sensation behind the breastbone)
Acid or food regurgitation
Chest discomfort not related to the heart
Sour or bitter taste in the mouth
Symptoms worse after meals or when lying flat
Some patients experience extra-oesophageal symptoms, such as:
Chronic cough
Hoarse voice
Throat clearing
Sensation of a lump in the throat
When Is Acid Reflux More Concerning?
Reflux should be assessed by a specialist if:
Symptoms persist despite medication
Symptoms interfere with sleep or daily activities
There is difficulty swallowing
There is unexplained weight loss
There is ongoing chest pain
There is anaemia or evidence of bleeding
These features do not mean something serious is present, but they do warrant proper assessment.
How Is Acid Reflux Diagnosed?
Diagnosis is based on a combination of symptoms, response to treatment, and investigations where appropriate.
Investigations may include:
Gastroscopy (OGD) to assess inflammation, ulcers, Barrett’s oesophagus or hiatal hernia
24-hour pH monitoring to measure acid exposure
Oesophageal manometry to assess oesophageal muscle function
Barium swallow to assess anatomy
Not all patients require all tests. Investigations are tailored to symptoms and planned treatment.
Treatment Options for Acid Reflux
Treatment follows a stepwise approach, starting with the least invasive options.
Lifestyle Measures
These can reduce symptoms but do not correct underlying anatomy:
Weight optimisation where appropriate
Avoiding late meals
Smaller meal portions
Reducing trigger foods and alcohol
Elevating the head of the bed
Medication
The most commonly used medications are:
Proton pump inhibitors (PPIs)
Acid-reducing or neutralising medications
Many patients respond well to medication. Some require long-term treatment.
When Medication Is Not Enough
Some patients continue to experience symptoms despite appropriate medication, or do not wish to remain on long-term medication.
In these situations, further assessment helps determine:
Whether reflux is truly present
Whether a hiatal hernia is contributing
Whether surgery is appropriate
Surgical Treatment for Acid Reflux
Surgery is not required for most patients, but can be appropriate in selected cases where:
Symptoms persist despite optimal medical treatment
A hiatal hernia is contributing to reflux
Objective tests confirm significant reflux
Medication causes side effects or is ineffective
Anti-reflux surgery
Anti-reflux surgery aims to restore the normal valve mechanism between the stomach and oesophagus.
This is usually performed laparoscopically (keyhole surgery) and may involve:
Repair of a hiatal hernia (if present)
Reinforcement of the lower oesophageal sphincter
Surgery is planned carefully after appropriate investigations.
What to Expect If Surgery Is Recommended
Surgery is performed under general anesthetic
Whether a hiatal hernia is contributing
It is not usually a day-case procedure
Most patients stay one night in hospital
Recovery is gradual, with temporary dietary adjustment
After surgery
No driving for 2 weeks
No lifting more than 2 kg (a full kettle) for 4 weeks
Gradual return to normal activities
Temporary swallowing discomfort may occur and usually settles
Benefits of Appropriate Reflux Surgery
In appropriately selected patients, surgery can:
Improve reflux symptoms
Reduce or stop the need for medication
Improve sleep and quality of life
Address anatomical causes of reflux
Outcomes depend on correct diagnosis, careful patient selection, and appropriate surgical technique.
Important Reassurance
Acid reflux is common
Many patients are managed without surgery
Surgery is only recommended when evidence supports benefit
Assessment and investigation guide safe decision making
Acid Reflux – Frequently Asked Questions
Common queries related to the Acid Reflux.
Is heartburn the same as acid reflux?
Do I need to take medication forever?
Why do I still have symptoms despite medication?
Is surgery better than medication?
Will surgery cure my reflux?
Is reflux surgery safe?
Will I still be able to swallow normally after surgery?
Can reflux cause long-term problems?
When should I seek specialist assessment?
Key Message for Patients
Acid reflux is treatable
Careful assessment matters
Treatment is individualised
Surgery is considered only when appropriate
Clear advice and follow-up are essential for good outcomes
Ready to Take Control of Your Acid Reflux?
If you're tired of dealing with acid reflux symptoms, it's time to take the next step. Book a consultation today to discuss your symptoms and explore personalised treatment options. Together, we can create a plan that helps you achieve long-term relief.
Contact me today to schedule your appointment and take control of your acid reflux treatment.
About Us
Consultant-led clinic providing expert surgical care with a focus on patient well-being.
Treatment for
Our Branches
Spire South Bank Hospital:
139 Bath Rd, Worcester, WR5 3YB, UK
©2026 EliteSurgix. All rights reserved